Feeling short of breath can have a big impact on your life. But there are people who can support you and things you can do yourself that can help you to manage breathlessness.
Understanding breathing
Most of the time we do not think about our breathing. We just do it automatically. But if you have an illness that causes breathlessness, it may become an effort.
Knowing a bit about how your lungs work can help you to understand why you feel breathless.
How we breathe
Our bodies need oxygen all the time. If our muscles do not get enough oxygen, we become breathless. The medical word for breathlessness is dyspnoea (also spelled dyspnea).
When we breathe in (inhale), air enters through our mouth or nose and goes into the windpipe (trachea). This makes our chest and lungs expand. When we breathe out (exhale), our lungs get smaller again.
A large muscle under the lungs called the diaphragm (dye-uh-fram) helps get air into the lungs and allows them to expand. We also have muscles between the ribs (intercostal muscles) that help the chest to expand and let air into our lungs.
When we’re relaxed and breathing is easy, we use the diaphragm and intercostal muscles to breathe. If you’re finding it harder to breathe, muscles in the shoulders and chest can help, but they get tired quickly.
All these things working together is called the respiratory (breathing) system.
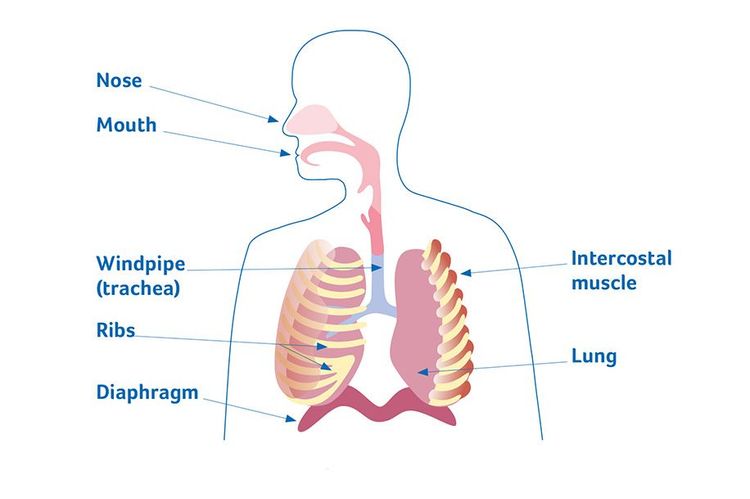
The respiratory system.
What is breathlessness (also called dyspnoea)?
Breathlessness, or shortness of breath, is an uncomfortable feeling of difficulty with breathing. It’s normal to feel breathless at times (for example, after hurrying for a bus). But breathlessness can also be caused by illness.
People’s experience of breathlessness can be different. Some people feel breathless all the time (constant breathlessness). For other people, it may come and go (episodic breathlessness). Breathlessness that develops over weeks or months is called long-term (chronic) breathlessness.
You might feel more breathless when you’re doing an activity, or if you’re feeling anxious. Or you might not know why you’re feeling breathless. Even with the right treatment, some people may still feel breathless.
How breathlessness can affect day-to-day life
Breathlessness can affect every part of your life and it can be difficult to deal with. You may feel breathless walking, getting dressed, climbing stairs, having a shower or doing housework.
If breathlessness is making it more difficult to do things you usually do, you might need to ask friends, family members and professionals for support.
Breathlessness can feel frightening. You might feel worried or panicky when you feel breathless (see What can you do to manage breathlessness? below).
What causes breathlessness?
Speak to your doctor or nurse if you feel breathless. They can find out what’s causing it and recommend the best ways to manage it. If there’s a reversible cause, like an infection, they can treat this.
Sometimes people still experience breathlessness after an illness has been treated. Tell your doctor or nurse if this happens to you, as there may be treatments that can help.
You can develop breathlessness if any part of your respiratory (breathing) system is not working properly. Click on the buttons below to find out possible reasons for this.
What can you do to manage breathlessness?
There are lots of things you can do that can help with breathlessness. You can try the suggestions on this page. And you may want to ask your doctor or nurse if there’s a breathlessness service in your local area.
We also have a free booklet with breathing techniques, medicines and other things that can help.
Try different breathing positions
Sitting, standing or lying in certain positions can make it easier to fill your lungs with air when you breathe in. Not every position works for everyone, but you can try them out and see what works best for you.
You can do these by yourself, or ask a physiotherapist, doctor or nurse for support. It can help to wear clothing that is loose around your waist or chest.
-
Sit upright in a chair with your back against the back of the chair and rest your hands on your thighs.
-
Sit on a chair leaning forward with your forearms resting on your thighs.
-
Sit or stand leaning forward with your arms resting on a ledge, for example a windowsill or table.
-
Lean back against a wall with your feet a comfortable distance from the wall and slightly apart. Relax your shoulders and let your arms hang down by your sides or rest them in your pockets.
-
If you’re in bed, try to lean back against a few pillows so you’re sitting upright. Or you can lie on your side with pillows under your head and shoulders. Make sure the top pillow supports your head and neck. A V-shaped pillow can be helpful.
Once you’re in one of these positions you can try breathing control techniques.
Breathing control techniques
Breathing control means using techniques to breathe gently, using as little effort as possible. They can help when you are short of breath or feeling anxious. These techniques can help let more air into your lungs, and help you feel more in control of your breathing.
You might find some of them work better than others. You can try them by yourself – of if you need any extra help, ask your physiotherapist, doctor or nurse. It can be helpful to practice these techniques when you’re not feeling breathless.
Pursed-lip breathing
Pursed-lip breathing is something you can try at any time, or while you’re doing something that makes you feel short of breath.
This is how to do pursed-lip breathing:
- Get into a comfortable position for your breathing (see Try different breathing positions above).
- Breathe in gently through your nose.
- Purse your lips as if you were going to whistle.
- Blow out with your lips pursed when you breathe out.
- Do this gently for as long as it feels comfortable.
- Do not force the air out of your lungs.
Blow as you go
This breathing control technique helps you to breathe more easily while doing activities. You can use it while you’re doing something that makes you breathless.
Blow as you go means:
- Taking a breath in just before you do something.
- Then breathing out while you’re doing it. It can be helpful to use pursed-lips when you blow out.
This can be useful for an activity that feels like an effort. For example:
- stretching your arms above your head to reach for something
- reaching or bending down
- lifting something heavy
- climbing stairs
- standing up.
Use a fan or open a window
A draught of cool air across your face can help you to feel less breathless. Using a fan with breathing exercises can help slow your breathing, and recover from an episode of breathlessness more quickly.
You could use a desk fan or a stand-up fan to create a draught of air in the room. Place the fan so the air hits one side of your face, just in front of your ear. You could also keep a small hand-held fan with you for when you need it.
If you’re inside, it can help to open a window as long as it’s not too cold for you.
Making the most of the energy you have
Following the five Ps is a way to make the most of your energy. The five Ps are: prioritising, planning ahead, pacing, positioning and permission.
Using this system can mean you don’t feel breathless as quickly when you’re doing an activity. It can be particularly helpful for people who have fatigue as well as breathlessness.
Make changes to how and what you’re eating
If you get breathless when you’re eating, these things might help:
- Take your time while you’re eating.
- Try softer, moist foods like soups, smoothies and pureed foods that are easier to chew and swallow.
- Sit down to eat and do not eat while you’re moving.
- Try not to talk while you are eating.
- Try eating smaller meals and having snacks throughout the day.
Try some physical activity
It can be hard to do physical activity if you have breathlessness. But keeping active can help improve your fitness and can actually help your breathing over time.
It’s best to plan an activity with breaks and rest periods before you do anything else. For example, if you’re walking to the shops in the morning, make sure you can rest in the afternoon.
Physical activity could include walking, gardening or swimming. Or it could be practising sitting to standing, or simply moving your arms and legs in a chair or in bed.
A physiotherapist can give you a programme of exercises designed for you. Some hospitals and hospices run exercise groups for patients who are breathless.
These are things to be aware of when you’re doing physical activity:
- You should still be able to talk in short phrases as you exercise. If you cannot do this, slow down until you get your breath back.
- Controlled breathing exercises can help manage your breathing while you exercise (see Breathing control techniques above).
- Plan ahead by thinking about where you could rest. For example, where there are walls or benches you could sit on. This may help if you feel anxious about finding somewhere to stop.
Becoming breathless when you’re exercising can be unpleasant, but it’s not usually harmful. It should settle after you rest for a few minutes.
Walking aids
Some people find that using a walking aid, like a wheeled walker, can help their breathing. This is probably because the way you lean forward and put pressure on your arms to use the aid, helps you get air into your lungs. If you’re finding it difficult to walk, it can also be a good way to continue to do physical activity. And this can help with your breathing more generally.
Using a walking aid can also mean you can stop for a rest without having to sit down and get back up again. And if using a walking aid means you can be more mobile, this may help with your confidence too.
You can ask your doctor, nurse or physiotherapist about using a walking aid.
Cut down or stop smoking
Smoking can make breathlessness worse. If you smoke and want support to stop or cut down, ask your doctor or nurse. They can discuss a range of different ways to help you to stop.
E-cigarettes (also called vapes) are thought to be less harmful than cigarettes. While we do not know their long-term effects, they may make symptoms of breathlessness worse.
Managing anxiety
If you have anxiety, it can help to talk about it with someone you trust. This could be a friend, family member or your doctor or nurse.
You can also contact our free Support Line on 0800 090 2309 or email support@mariecurie.org.uk for practical information and emotional support.
Your doctor or nurse can prescribe medicines to help, and they may refer you to a different professional for more support. This could be a counsellor or psychologist, who can help you understand and work through your feelings.
Counselling is a talking therapy that is sometimes free at hospices, hospitals or GP surgeries. Your doctor or nurse can let you know what talking therapies are available locally, and can help you decide which treatment is best for you. Speak to your GP for more information about free counselling services.
You may also be able to get private counselling, which you would need to pay for. For more information, ask your doctor. Or, visit the British Association of Counselling and Psychotherapy website to find a qualified counsellor near you.
Breathing techniques
These techniques can help get your breathing under control if you feel anxious or panicky. Try practicing them so you’re ready to use them if you do start to feel short of breath or anxious.
Rectangular breathing
Imagine a rectangle. Or you can look at a rectangle in the room, like a TV screen or picture frame.
- Breathe in and imagine going up one side of the rectangle.
- Breathe out and imagine going along the top of the rectangle.
- Breathe in and imagine going down the other side of the rectangle.
- Breathe out and imagine going along the bottom of the rectangle.
Keep breathing in and out in this way until your breathing feels under control.
Try to increase how long you breathe out. You could start by trying to breathe in for three seconds and breathing out for five seconds.
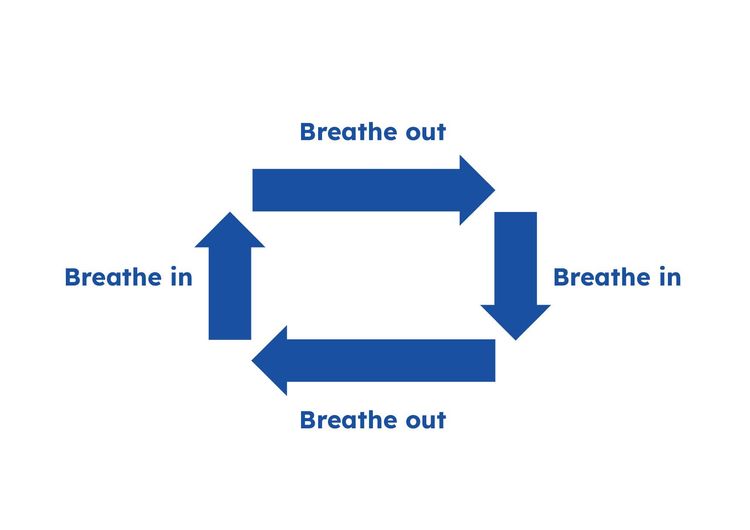
Rectangular breathing technique
Square breathing (box breathing)
- Breathe in slowly for four seconds. Be aware of how the air fills your lungs and stomach.
- Hold your breath for four seconds.
- Exhale for four seconds.
- Hold for four seconds.
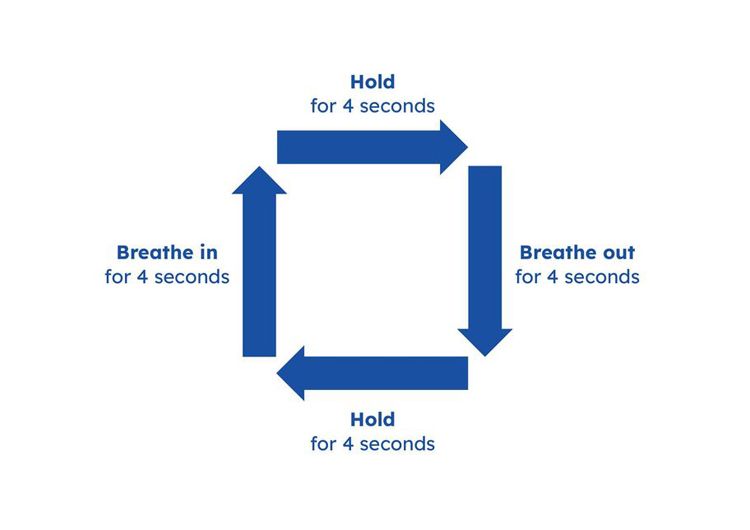
Square breathing technique
It’s fine if you find it more comfortable to breathe in for shorter or longer than four seconds. The important thing is that you breathe in and out for the same length of time. Keep doing this until your breathing feels under control.
For both rectangular breathing and square breathing – ideally breathe in through your nose, and out through your mouth. But this might not be possible for everyone – do what feels most comfortable for you.
Relaxing
Finding ways to relax may help you manage breathlessness and anxiety. Try to find time for relaxation each day. This could include breathing exercises, or listening to music or an audiobook. Or could might like to spend time outside, have a bath, or try meditating.
Complementary therapies
Some people find complementary therapies like acupuncture, reiki, and massage make them feel more relaxed, which can help with their breathlessness.
Speak to your doctor or nurse before trying a complementary therapy. They can advise what’s suitable and safe for you, depending on your health condition and treatment.
It’s also important to tell the complementary therapist about your medical condition, and any treatments you’ve had or are having. They can make sure the therapy is suitable for you.
Some complementary therapies are free on the NHS, but they’re not always available. Speak to your doctor or nurse about what’s available in your area. Your local hospice or a local support group may also offer free or reduced cost therapies. You can also get complementary therapies privately, but you will have to pay for these. Private therapists can be expensive, so it’s worth checking the cost first.
Medicines for breathlessness
There are different medicines that can help with breathlessness:
- Medicines to treat the illness that’s causing your breathlessness.
- Medicines to help reduce the feeling of breathlessness.
Ask your doctor or nurse about the best medicines for you.
Medicines for an illness causing breathlessness
Medicines that help reduce the feeling of breathlessness
Breathlessness diary and action plan
It can be helpful to keep a diary of when you feel breathless. This can help you see if it’s worse at certain times, or after particular activities. And it can help you plan activities for when you have more energy, and make the most of the energy that you have.
You may also want to use the action plan. This a place to write down the techniques and medicines that work well for you.
Professionals who can support you
If you need help to manage your breathlessness, there are lots of professionals who can support you. Your GP, hospital team or local hospice can refer you to other professionals.
Breathlessness towards the end of life
Breathlessness can affect people at any stage of their illness. Sometimes, breathlessness can get worse as someone’s illness progresses and they near the end of their life.
People can still use the techniques they’ve found helpful, such as controlled breathing and using a fan, if it’s comfortable.
Someone’s breathlessness may improve for a while as they’re less able to do activities and need to rest more. There are medicines that can keep someone comfortable even as they become more breathless. A doctor or nurse can help with medicines if breathlessness becomes more difficult to manage.
Supporting someone with breathlessness
There are lots of ways you can support someone experiencing breathlessness. It can help to understand that your relationship with them might change if you need to take on more tasks.
- Find out what they want to do themselves.
- Support them to do those activities at their own pace.
- If you need extra help with tasks like cooking and cleaning, speak to the person’s doctor or social worker, if they have one. A clinical nurse specialist in palliative care may be able to help with the forms you need to claim for these costs.
- See if they would like help with breathing exercises and relaxation techniques.
- Ask if they would like you to go with them to appointments, or sessions about managing breathlessness. This might make it easier for you to help them with the techniques.
- Keep rooms well-ventilated by opening windows or using a fan.
- Let them know they can talk to you about any fears or worries they may have.
Supporting someone with breathlessness due can be rewarding, but also challenging. If you need support, speak to your GP. They can support you with your own health, refer you to a social worker, or recommend local support groups.
Getting support
If you would like to speak to someone, you can call our free Support Line on 0800 090 2309 or email support@mariecurie.org.uk They can provide emotional support, or you can speak to an Information and Support Nurse if you'd like practical information.
Marie Curie's Online Community can be a place to connect with others living with breathlessness, or caring for someone who has this symptom.

